Understanding Fluid, Electrolyte, And Carbohydrate Replacement During Activity
G. Douglas Andersen, DC, DACBSP, CCN
Natural Medicine Journal, Volume 9, Number 9, November 1998
Exercise and activity are something most physicians routinely recommend. This article will give the clinician an overview of the physiology of exercise in the heat, intestinal absorption of fluid. Specific types of carbohydrates and electrolytes, and their importance in a rehydration beverage will also be discussed. Recommendations from the American College of Sports Medicine and this author are also included.
Heat Physiology During Exercise
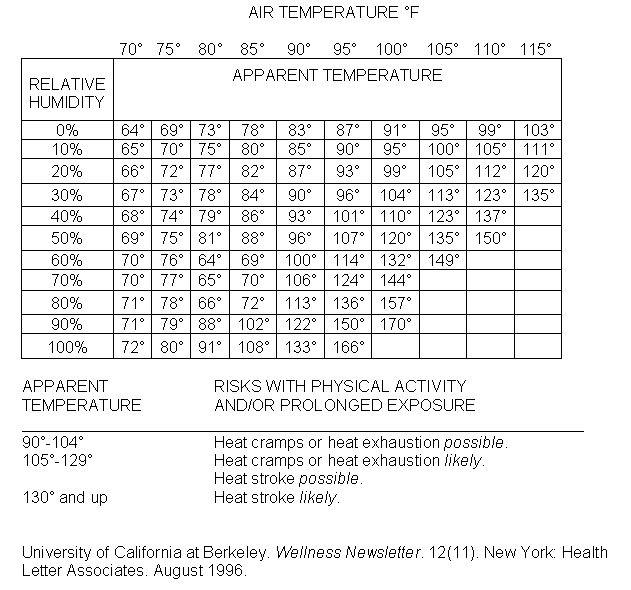
Heat stress is a combination of temperature, humidity, wind, and thermal radiation. The heat index is composed
of a combination of air temperature and relative humidity. This yields the apparent temperature, which can
then be used by the clinician to assess the risks of activity with prolonged exposure (see Table I). During
rest, 60% of heat loss is from radiation, 20% from conduction and convection, and 20% from evaporation. During
exercise, 80% of heat loss is from evaporation with conduction and convection making up 15%, and only 5% coming
from radiation. At rest the body produces 1.5 kcal of heat per minute. During exercise (70% V02 max) 15 kcal
per minute of heat is produced. When exercise is performed in hot conditions, the body requires greater
oxygen uptake than when it is cool. This leads to an increase of internal heat production, increased heart
rate, increased glycogen utilization, increased acid production, and a decrease in the time to fatigue.1
A good example of how temperature affects performance is demonstrated in a study by Galloway and Maughan.2 They studied the time to fatigue of fully hydrated subjects riding exercise bikes at moderate intensities under various Fahrenheit temperatures. At 52 degrees subjects were able to ride for 92 minutes. At 70 degrees the average was 83 minutes. At 86 degrees fully hydrated subjects were able to ride for only 51 minutes before their intensity dropped below the assigned level.
Effects of Humidity
Exercise and activity in hot, humid conditions poses the greatest risk for heat-related illness. Air saturated
with water molecules has a decreased capacity to accept sweat. When less sweat evaporates, body temperature
rises which, in turn, places additional stress on all systems. When humidity is 60% or more, sweat evaporation
stops unless there is air movement.3 With high humidity, the thirst mechanism is inhibited due to the fact
that the throat is not dry.
Hot and very dry conditions can also cause heat-related illness. In desert-like environments, sweat evaporates so rapidly that people do not realize how much fluid they are losing. When the weather is hot and very dry, it can give unacclimated persons the perception that the temperature is cooler than it really is. This combination of perceived temperature moderation with the appearance of only light sweating can fool the unprepared person regarding the danger he or she potentially faces.
Sweat Rates
There is marked individual variability of sweat rates during exercise. Factors that affect water balance
during activity include:
- Individual metabolism. Most adults are aware if they are heavy or light sweaters.
- Type of event. Sweat rates are greater when an event is performed with higher intensity and/or longer duration.4
- Ability to consume fluid during the event.
- Temperature. Higher temperatures, higher humidity, and lower wind speed will all increase the amount of fluid lost.4
- The level of fitness. Better physical fitness results in a more efficient sweat response as core temperature increases during activity. Generally, individuals will sweat more.5
- Pre-event hydration level. Dehydrated people will sweat less which, in turn, will cause an increase in core temperature.
- Acclimatization. Heat acclimatized people will start sweating at lower temperatures and will lose a greater amount of sweat than the unacclimatized person, and thus will be able to keep their bodies cooler. Full acclimatization takes seven to fourteen days, although the body will begin the adapting process immediately.6
- Body surface area. Individuals with greater body surface area will lose more fluid.
- Gender and age. Males will generally sweat more than females, and adults will sweat more than children and teenagers.7
Fluid Losses
A normal sedate person in a temperate climate loses two liters of fluid per day. The major avenues of loss
include sweat, urine, respiration, and feces. A normal sedate person in a hot and/or humid climate can lose
four to six liters of fluid per day.8 Athletes or those active in hot and humid conditions can lose one to
three liters of fluid per hour.9 For an athlete who is training hard in a hot climate for three hours a day,
the daily water turnover can range from five to ten liters with requirements as high as fifteen liters in
extreme conditions.8 See Tables II and III for the Adverse Effects of Water Loss and Physiologic Responses
to Dehydration.
| PERCENT WEIGHT LOSS | OBSERVED EFFECTS |
| 1 | Threshold for thirst and for impaired exercise thermal regulation leading to decrement in work capacity |
| 2 | Stronger thirst, vague discomfort and sense of oppression, loss of appetite |
| 3 | Dry mouth, increasing hemo concentration, reduction in urinary output |
| 4 | Decrement of 20-30% in physical work capacity |
| 5 | Difficulty in concentrating, headache, impatience, sleepiness |
| 6 | Severe impairment in exercise temperature regulation, increased respiratory rate leading to tingling and numbness of extremities |
| 7 | Likely collapse if combined with heat and exercise |
| 1 | Reduced rate of gastric emptying. |
| 2 | Increased incident of gastric distress. |
| 3 | Increased plasma angiotensin and vasopressin. |
| 4 | Decreased splanchnic and renal blood flow. |
| 5 | Decreased plasma volume. |
| 6 | Decreased plasma osmolality. |
| 7 | Increased blood viscosity. |
| 8 | Decreased central blood volume. |
| 9 | Decreased central venous pressure. |
| 10 | Decreased cardiac filling pressure. |
| 11 | Decreased cardiac stroke volume. |
| 12 | Increased heart rate. |
| 13 | Decreased cardiac output. |
| 14 | Decreased sweat rate and skin blood flow. |
| 15 | Decreased maximal skin blood flow. |
| 16 | Increased body temperature before sweating and skin blood flow increase. |
| 17 | Increased core temperature. |
Carbohydrates
In the last few years the consensus range of the percent of carbohydrates contained in a fluid-replacement
beverage consumed during competition had been 4-8%.10 Recently, this range appears to be shrinking with
evidence pointing to optimal levels in the 6-7% range, with at least two carbohydrate sources.11 Finally,
it is well accepted that the consumption of carbohydrates during prolonged activity will improve
performance.5,12,13,14,15,16,17
Glucose
Glucose is one of the most common carbohydrate sources in sports drinks. All carbohydrates must be converted
to glucose by the liver before they can be utilized as fuel by skeletal muscle. Glucose stimulates the
absorption of sodium and water.18
Glucose Polymers
Glucose polymers are also known as maltodextrin, and are popular in sports drinks. Glucose polymers have a
20% lower osmotic pressure than glucose. This lower value theoretically increases the rate of gastric
emptying, decreases the movement of fluid from plasma to the interstitial lumen, and decreases the rates of
gastric secretion.19 Other studies have shown that when glucose polymers are consumed during exercise there
is no difference in the rate of gastric emptying, intestinal carbohydrate delivery, or carbohydrate oxidation
when compared to glucose solutions.20
Fructose
Fructose has a glycemic index of 23 using glucose as a reference of glycemic index of 100.21 When fructose is
the only carbohydrate source in a beverage, the oxidation ratio is slow; thus, the conversion to usable
substrate (glucose) is also slow. For exercising athletes, this is not a benefit.22 In some people, when large
quantities of fructose are ingested during exercise, gastrointestinal distress may be provoked.23,24 Fructose is
well tolerated when taken with equal amounts of glucose or when taken in as sucrose.25 If the ratio of
fructose to glucose exceeds one, fluid uptake can be inhibited.26 At a ratio of one or less, the simultaneous
intake of fructose and glucose can generate an osmotic pressure that will increase the absorption of water
across the intestines5 (assuming the total percent of carbohydrate is no greater than eight).
Sucrose
The literature is divided regarding the ability of sucrose to promote glucose and water absorption in exercise
in humans.27 Sucrose as an ergolytic substance is not supported in the peer-reviewed literature although it
continues to have a bad reputation in the health food community. Sucrose, along with glucose and glucose
polymer, appear very similar in the ability to delay fatigue and enhance performance.28,29
Glycemic Index
Glycemic index and its effect on exercise is a relatively new area of scientific study. Thus, the body of
literature at present is limited when compared to other areas concerning energy and exercise. Based on what
is known, low glycemic foods or beverages (including fructose, proteins, and fats) when consumed 30 to 60
minutes prior to exercise tend to minimize exercise-induced hypoglycemia when an activity is initiated. Low
glycemic index foods also tend to promote the use of lipids as fuel.
Ingestion of highly concentrated beverages (90 calories or more per eight ounces) just prior to or in the early stages of exercise may, in some people, adversely affect performance in two ways. The first is by decreasing the rate of fluid absorption caused by the high concentration of the solution. The second is by depressing the oxidation of fat for fuel and accelerating the oxidation of carbohydrate, which in long events may lead to premature fatigue.27 Ingestion of beverages with not enough carbohydrates (less than 4%) may also reduce performance in the late stages of endurance events due to inadequate carbohydrate intake.30 There is conflicting data on whether the consumption of low glycemic index foods will improve performance.31,32
During exercise, foods and beverages with a high glycemic index will affect the body differently than at rest. Activity-induced epinephrine release reduces insulin secretion. When muscles are exercising, less insulin is required to deliver glucose to target tissues.1
Following exercise, the consumption of high glycemic index foods will replenish glycogen faster, especially in the first five hours after activity, than foods whose glycemic index is lower. Furthermore, when glycogen levels are depleted, foods with higher glycemic indexes will not cause blood glucose or insulin to rise as much as they would with normal glycogen levels. Thus, the glycemic index of foods can vary depending on the glycogen content of tissues.33
Digestive Physiology
The digestive physiology for fluid, carbohydrate, and electrolyte replacement can be divided into two phases,
gastric emptying and intestinal absorption. Gastric emptying is not a linear process. There are fast and
slow phases as well as marked individual variability in the speed of gastric emptying.34 Gastric volume has
the greatest influence on gastric emptying. Increased volumes up to at least 600 ml will increase gastric
emptying.35 Other factors that influence gastric emptying include the carbohydrate and mineral contents of a
solution, as well as its temperature. Cooler, flavored beverages stimulate fluid intake.36,37 Exercise at
high intensity can also affect gastric emptying. Exercise below 70 V02 max will not delay gastric emptying.38
Intestinal Absorption
Little fluid is absorbed from the stomach.39 Fifty to sixty percent of fluid absorption occurs in the small
intestine, and 1.9 to 2.3 liters per hour is the maximum that can be absorbed.40 Carbohydrates do stimulate
sodium and fluid absorption in humans.41 Sodium is required for, and chloride enhances, fluid
absorption.40 More fluid is absorbed from a carbohydrate electrolyte beverage than from plain
water, both at rest and during exercise as long as the carbohydrate content is not too high.40 Solutions
formulated with two or more carbohydrates stimulate more water absorption even though combining different
substrates increases the solution osmolality. Different substrates overcome the increased osmolality by
stimulation of multiple transport mechanisms.42 Sodium-containing fluids result in a greater percentage of
fluid retained in dehydrated athletes; i.e., athletes will rehydrate faster with less urinary excretion.8 There
are no physiologically important differences in the rates of carbohydrate oxidation from a
variety of mono-, di-, and polysaccharides ingested during exercise. All are ultimately oxidized at a rate of
approximately 1/3 gm per minute for the first 60 minutes.18 This rate increases to approximately 1 gm per
minute after 70-90 minutes of exercise.43
Electrolytes
Sodium
Sodium chloride has many important functions for the exercising individual. When included in a rehydration
beverage, sodium chloride promotes carbohydrate and fluid absorption. It improves taste, stimulates thirst,
and maintains plasma volume during exercise by decreasing urine production.44,45 Many commercial sports drinks
may lack optimal amounts of sodium. For example, Gatorade contains 21 mEq of sodium, which converts to
approximately 450 mg per liter. Although the sodium content of Gatorade is higher than most commercial sports
drinks, it is still below the amount recommended by the American College of Sports Medicine position stand
in 1996.
If an athlete consumes more sodium than he or she loses, the excessive consumption of sodium generally will have no detrimental effects on health, provided that fluid intake exceeds sweat losses and the kidneys are functionally normally.
The range of sodium in sweat is 30-110 mmol per liter with typical sweat values at 50 mmol. Sodium is the main ion lost in sweat.8,39 Sodium is required for, and along with chloride enhances fluid absorption.40 One liter of sweat at a sodium concentration of 50 mmol per liter equates to 2.9 gm of sodium chloride.8 Sodium is by far the most important electrolyte to be included in a sports drink. Because the average U.S. intake of sodium chloride ranges from 2-9 gm per day,9 many scientists and physicians have recommended that the inclusion of sodium is not important in a fluid-replacement beverage. However, when considering that an average of 2.9 gm of sodium chloride can be lost in a liter of sweat,8 individuals performing heavy activity in the heat can theoretically lose 5000 to 9000 mg of sodium chloride per hour. Tennis players have been measured to lose sodium at a rate of 2000-5000 mg per hour.46,9
An example of the continuing confusion regarding sodium is best exemplified in Chapter 34, entitled "Fluid Balance" by Cushner and Cushner in the book Sports Medicine Principles and Primary Care by Scuderi, McCann, and Bruno, Moseby, 1997, page 574. On that page the authors include a table which recommends the inclusion of sodium chloride in fluid-replacement beverages for activities lasting longer than one hour to promote carbohydrate and fluid absorption and enhance palatability. On the same page the authors ask "Is the inclusion of sodium necessary in these events? (One to three hours)." The answer is probably "No." In my experience treating professional beach volleyball players, the answer to this question would be "Yes" for 10% of the athletes competing in normal summertime conditions (80 degrees with average humidity). As the temperature and humidity increase, the percent of players who require sodium also increases. In very hot and humid weather (over 90 degrees and 70% humidity), it is my experience that 75% of professional beach volleyball players will require extra sodium ranging from 1000-4000 mg per hour along with adequate fluids to avoid heat-related illness.
Potassium
Typical sweat volumes of potassium are 5 mmol per liter with a range of 2.5-9.3 mmol per liter. Sweat that
contains 5 mmol per liter of potassium amounts to 200 mg of potassium.8 The risk for potassium deficiency
during exercise is increased with diuretic use.44 Potassium facilitates rehydration of the intracellular
fluid compartment.47 Three to five milliequivalents per liter (approximately 100-200 mg per liter) is
recommended for inclusion in a sports drink.44
Magnesium
It is highly unlikely that sweat losses can trigger hypomagnesemia,48 although the risk does increase for those
using diuretics.44 Because magnesium is so important in so many reactions, a small amount included in a sports
drink is not detrimental, although there is no evidence of performance enhancement in individuals who do not
have a magnesium deficiency.
Chromium
Exercise increases plasma chromium via mobilization of muscle tissue. Physical activity increases chromium
turnover and promotes its loss through the urine.49 Chromium utilization and losses increase in a
linear fashion with total work load.49
Recovery
Most athletes progressively voluntarily dehydrate throughout their competition or event.50 Athletes will seldom
consume more than 16 ounces of fluid per hour during exercise which is often considerably less than sweat
rates.51 Athletes will commonly stop drinking before they are fully hydrated after exercise.51 The first two
hours of rehydration have a marked influence on the rate of recovery and performance in subsequent athletic
events on the same day.27 Consuming 100% of the fluid lost will not fully rehydrate a person because urine
production can be as high as a half liter per hour following rehydration.52 Existing data shows that athletes
must consume at least 150% of weight loss within six hours post exercise to fully rehydrate. Some cases will
require fluid replacement at the 2:1 ratio.52 Merely drinking a large volume of beverage after
exercise-induced dehydration is not sufficient to achieve complete rehydration if the sodium concentration is
inadequate.52 Ingesting a beverage with a high sodium concentration is not sufficient to achieve rehydration
if the volume consumed is not appropriate.52 Drinking by thirst alone will take at least 24 hours to fully
rehydrate, and this assumes the day is spent in a sedate manner and in a temperate climate, and meals have been
consumed.1 There are many studies which show that people will consume larger amounts of solutions that have a
favorable flavor.8
The American College of Sports Medicine's 1996 Position Stand on Fluid Replacement53
- Drink at least 500 ml (17 ounces) two hours prior to event or activity.
- During exercise drink at a rate that equates to fluid loss or as much as one comfortably can.
- Fluids should be cool (15-22°F or 59-72°F) and flavored to promote consumption.
- Carbohydrates and electrolytes should be in beverages for events that last longer than one hour.
- In events of intense exercise greater than one hour, carbohydrates should be ingested at a rate of 30-60 gm per hour. This can be accomplished by drinking 600-1200 ml of solutions that contain 4-8% carbohydrate (a sports drink at a 6% carbohydrate level will contain approximately 60 gm of carbohydrate per liter).
- The recommended carbohydrate sources in a sports drink are glucose, sucrose, or maltodextrin.
- For exercise longer than one hour, sodium at 500 700 gm per liter should be included in a fluid-replacement beverage.
Recommendations
- Counsel patients to drink before they are thirsty. Inform them that the more they drink the more they will absorb, and that the rule of thumb should be to consume as much as they comfortably can.
- During activity the consumption of sports drinks that contain carbohydrates and electrolytes is perferred over water.
- Sports drinks should contain 50-70 calories per eight ounces using two or more types of carbohydrates, along with adequate sodium (100 mg or more per eight ounces) and potassium (25 mg or more per eight ounces). The inclusion of additional minerals is optional.
- Advise patients that small amounts of dark-colored urine indicate that they are dehydrated and they should immediately increase their fluid intake.
- Often overlooked is the fact that when a person does get dehydrated, the gastric emptying rate is reduced; thus, rehydration will take longer.
- The guideline of fluid replacement which was to consume a pint of fluid per pound of body weight loss after activity is inadequate for persons who will be involved in additional competition within a 24-hour period. For these athletes, rehydration should be practiced at the level of 20-24 ounces of fluid per pound of lost body weight.
- Advising athletes and active people prone to heat-related illness to increase their sodium consumption during active years should be done with the realization that this could potentially set up dangerous eating patterns in future noncompetitive years.
- There is a growing body of evidence which indicates that consuming sports drinks during intermittent, intense activities (stop-start sports) of less than one hour can improve performance. Most of this work was published after the 1996 ACSM guidelines.54,55,56,57,58
- For the exercising athlete, consuming beverages containing sucrose and sodium during competition is not unhealthy. This should not be confused with excessive sucrose and sodium consumption of sedate and unfit individuals.
References
1Wilmore, J., and D. Costell. Physiology of Sport and Exercise. Human Kinetics. 1994.
2Galloway, S. D. R., and R. J. Maughan. Effects of Ambient Temperature on Capacity to Perform Exercise in Men. Journal of Physiology. 489:35-36. 1995.
3Scuderi, McCann, and Bruno. Sports Medicine Principles of Primary Care. Moseby. 568-577. 1997.
4Sawka, M.N., and K.B. Pandolf. Effects of Body Water Loss in Physiological Function and Exercise Performance in Perspectives. From Exercise Science and Sports Medicine: Fluid Homeostasis During Exercise, D. R. Lamb and C. V. Gisolfi. Indianapolis, Ind.: Benchmark Press. 1990.
5Horswill, C. Effect of Fluid Replacement. International Journal of Sport Nutrition. 8(2):175-195. June 1998.
6Maughan, R. J., and S. M. Shirreffs. Preparing Athletes for Competition in the Heat: Developing an Effective Acclimatization Strategy. Sports Science Exchange. 10(2). 1997.
7Meyer, F., et al. Sweat Electrolyte Loss During Exercise in the Heat: Effects of Gender and Maturation. Medicine and Science in Sports and Exercise. 24:776-781. 1992.
8Maughan, R. J., J. B. Leiper, and S. M. Shirreffs. Rehydration and Recovery after Exercise. Sports Science Exchange. 9(3). 1996.
9Mack, G. W., and M. F. Bergeron. Hydration and Physical Activity: Scientific Concepts and Practical Applications. Sports Science Exchange. 7(4). 1996.
10Coyle, E. F., and S. J. Montain. Benefits of Fluid Replacement with Carbohydrate During Exercise. Medicine and Science in Sports and Exercise. 24(S9):S324-S330. 1992.
11Shi, X., et al. Effects of Carbohydrate Type and Concentration and Solution Osmolality on Water Absorption. Medicine and Science in Sports and Exercise. 27:1607-1615. 1995.
12Murray, R., D. E. Eddy, et al. The Effect of Fluid and Carbohydrate Feeding During Intermittent Cycling Exercise. Medicine and Science in Sports and Exercise. 19:597. 1987.
13Davies, J. M., D. R. Lamb, et al. Carbohydrate Electrolytes Drinks; Effects on Endurance Cycling in the Heat. American Journal of Clinical Nutrition. 48:1023. 1988.
14Murray, R., G. L. Paul, et al. The Effects of Glucose, Fructose, and Sucrose Ingestion During Exercise. Medicine and Science in Sports and Exercise. 21:275. 1989.
15Millard-Stafford, M., P. B. Sparling, et al. Carbohydrate-electrolyte Replacement During a Simulated Triathlon in the Heat. Medicine and Science in Sports and Exercise. 22:621. 1990.
16Murray, R., G. L. Paul, et al. Responses to Varying Rates of Carbohydrate Ingestion During Exercise. Medicine and Science in Sports and Exercise. 23:713. 1991.
17Febbraio, M.A., P. Murton, et al. Effect of Carbohydrate Ingestion on Exercise, Metabolism, and Performance in Different Ambient Temperatures. Medicine and Science in Sports and Exercise. 28:1380-1387. 1986.
18Johnson, H. L. Requirements for Fluid Replacement During Heavy Sweating and the Benefits of Carbohydrates and Minerals. From Sports Nutrition: Minerals and Electrolytes, C. Kies. Boca Raton, FL: CRC Press. 1995.
19Wheller, K., and J. G. Banwell. Intestinal water and electrolyte flux of glucose polymer electrolyte solutions. Medicine and Science in Sports and Exercise. 18:436. 1986.
20Rehrer, N. J., et al. Gastric Emptying, Absorption, and Carbohydrate Oxidation During Prolonged Exercise. Journal of Applied Physiology. 72:468. 1992.
21Foster-Powell, K., J. Brand Miller. International Tables of Glycemic Index. American Journal of Clinical Nutrition. 62:871-893S. 1995.
22Massicotte, D., F. Perronnet, et al. Metabolic Response to Glucose and Fructose Ingestion During Exercise. Journal of Applied Physiology. 61:1180-1184. 1986.
23Murray, R. Fluid Replacement. Sports Science Exchange. 9:4. 1996.
24Fruth, J. M., and C. V. Gisolfi. Effects of Carbohydrate Consumption on Endurance Performance: Fructose Versus Glucose. From Nutrient Utilization During Exercise. Ed. E.L. Fox. Columbus, OH: Ross Laboratories. 68-75. 1983.
25Rumessenn, J. J., and E. Gudmand-Hoyer. Absorption Capacity of Fructose in Healthy Adults: Comparison with Fructose and its Constituent Monosaccharide. GUT. 27:1161-1168. 1986.
26Schedl, H. P., R. J. Maughan, and C. V. Gisolfi. Intestinal Absorption During Rest and Exercise: Implications for Formulating and Oral Rehydration Solution. Medicine and Science in Sports and Exercise. 26-3:267-280. 1994.
27Gisolfi, C. V., and S. M. Duchman. Guidelines for Optimal Fluid Replacement Beverages for Different Athletic Events. Medicine and Science in Sports and Exercise. 24:679-687. 1992.
28Saris, W. H. M., B. H. Goodpaster, et al. Exogenous Carbohydrate Oxidation from Different Carbohydrate Sources During Exercise. Journal of Applied Physiology. 75:2168-2172. 1993.
29Wagenmakers, A. J. M., F. Brouns, W. H. M. Saris, and D. Halliday. Oxidation Rates of Orally Ingested Carbohydrate During Prolonged Exercise in Men. Journal of Applied Physiology. 75:2774-2780. 1993.
30Hawley, J. A., S. C. Dennis, and T. D. Noakes. Carbohydrate Fluid Electrolyte Requirements During Prolonged Exercise. From Sports Nutrition, Minerals, and Electrolytes, C. Kies. Boca Raton, FL: CRC Press: 1995. 235-65.
31Thomas, D. E., J. R. Brotherhood, and J. C. Brand. Carbohydrate Feeding Before Exercise: Effect of Glycemic Index. International Journal of Sports Medicine. 112:180-186. 1991.
32Thomas, D. E., J. R. Brotherhood, and J. Brand Miller. Plasma Glucose Levels After Prolonged Strenuous Exercise Correlate Inversely with Glycemic Response to Food Consumed Before Exercise. International Journal of Sports Nutrition. 4:361-373. 1994.
33Rankin, J. W.. Glycemic Index and Exercise Metabolism. Sports Science Exchange. 10(1). 1997.
34Minami, H., and R. W. McCallum. Physiology and Pathophysiology of Gastric Emptying in Humans. Gastroenterology. 86:1592-1610. 1984.
35Mitchell, J. B., and K. W. Voss. Influence of Volume on Gastric Emptying and Fluid Balance During Prolonged Exercise. Medicine and Science in Sports and Exercise. 23:310-319. 1991.
36Hubbard, R. W., B. L. Sandick, et al. Voluntary Dehydration and Allesthesia for Water. Journal of Applied Physiology. 57(3):868-875. 1984.
37Sandick, B. L., D. B. Engell, and O. Maller. Perception of Water Temperature and Effects for Humans after Exercise. Physiology and Behavior. 32:851-855. 1984.
38Brouns, F., et al. Abdominal Complaints in Gastrointestinal Function During Long-lasting Exercise. International Journal of Sports Medicine. 8:175-189. 1987.
39Guyton, A. C. Textbook of Medical Physiology, 6th Ed. Philadelphia: W. B. Saunders. 820. 1981.
40Gisolfi, C. V. Exercise, Intestinal Absorption and Rehydration. Sports Science Exchange. 4(32). May 1991.
41Schedl, H. P., and J. A. Clifton. Solute and Water Absorption by the Human Small Intestine. Nature. 199:1164-1267. 1963.
42Shi, X., H. P. Summers, et al. Effects of Carbohydrate Type and Concentration in Solute Osmolality on Water Absorption. Medicine and Science in Sports and Exercise. 27:1607-1615.
43Hawley, J.A., S. C. Dennis, and T. D. Noakes. Oxidation of Carbohydrate Ingested During Prolonged Endurance Exercise. Sports Medicine. 14:27. 1992.
44Cushner, G. B., and F. D. Cushner. Fluid Balance. From Sports Medicine Principles and Primary Care, Scuderi, McCann, and Bruno. Moseby. 1997.
45Neilson, B., et al. Fluid Balance and Exercise Dehydration and Rehydration with Different Glucose Electrolyte Drinks. European Journal of Applied Physiology. 55:318-325. 1986.
46Bergeron, M. F., L. E. Armstrong, and C. M. Maresh. Fluid and Electrolyte Losses during Tennis in the Heat. Clinical Sports Medicine. 14:22-3. 1995.
47Nadel, E. R., G. Mack, and H. Knows. Influence of Fluid-Replacement Beverages on Body Fluid Homeostasis during Exercise and Recovery. In Perspectives in Exercise, Science, and Sports Medicine, C. V. Gisolfi and D. R. Lamb, eds. Carmel: Benchmark Press. 1990. 181-205.
48Squire, D. L. Heat Illness: Fluid and Electrolyte Issues for Pediatric and Adolescent Athletes. Ped. Clin. N. Am. 37:1085-1109. 1990.
49Campbell, W. W., and R. A. Anderson. Effects of Aerobic Exercise and Training on Trace Minerals Chromium, Zinc, and Copper. Sports Medicine. 4(9). 1987.
50Noakes, T. D., B. A. Adams, et al. Danger of Inadequate Water Intake During Prolonged Exercise. European Journal of Applied Physiology. 57:210-219. 1988.
51Noakes, T. D. Fluid Replacement During Exercise. Exercise Sports Science Review. Holloszy, J.O., ed. Baltimore: Williams and Wilkins. 21:297-330. 1993.
52Shirreffs, S. M., et al. Postexercise Rehydration Level in Man: Affects of Volume Consumed and Drink Sodium Content. Medicine and Science in Sports and Exercise. 28:1260-1271. 1996.
53Medicine and Science in Sports and Exercise. 1996. 28(1): vii.
54Wagenmakers, A. J. M., et al. Carbohydrate Feedings Improve One Hour Timed Trial Cycling Performance. Medicine and Science in Sports and Exercise. 28:S37. 1996.
55Nicholas, C. W., et al. Influence of Ingesting a Carbohydrate Electrolyte Solution on Endurance Capacity During Intermittent High Intensity Shuttle Running. Journal of Sports Science. 13:283-290. 1996.
56Ball, T. C., et al. Periodic Carbohydrate Replacement During 50 Minutes of High Intensity Cycling Improves Subsequent Sprint Performance. International Journal of Sports Nutrition. 5:151-158. 1995.
57Below, P. R., et al. Fluid and Carbohydrate Ingestion Independently Improved Performance During One Hour of Intense Exercise. Medicine and Science in Sports and Exercise. 27:200-210. 1994.
58 Davis, J. M., D. A. Jackson, et al. Carbohydrate Drinks Delay Fatigue During Intermittent High Intensity Cycling in Active Men and Women. International Journal of Sports Nutrition. 7:261-273. 1997.
916
E. Imperial Hwy.
Brea, CA. 92821
(714) 990-0824
Fax:
(714) 990-1917
gdandersen@earthlink.net
www.andersenchiro.com
Copyright
2004, G. Douglas Andersen, DC, DACBSP, CCN, 916 E. Imperial Hwy, Brea,
CA 92821, (714) 990-0824